
Glycemic Optimization and Management of a Non-Healing Diabetic Foot Ulcer in a 55-Year-Old Male with Uncontrolled Type 2 Diabetes
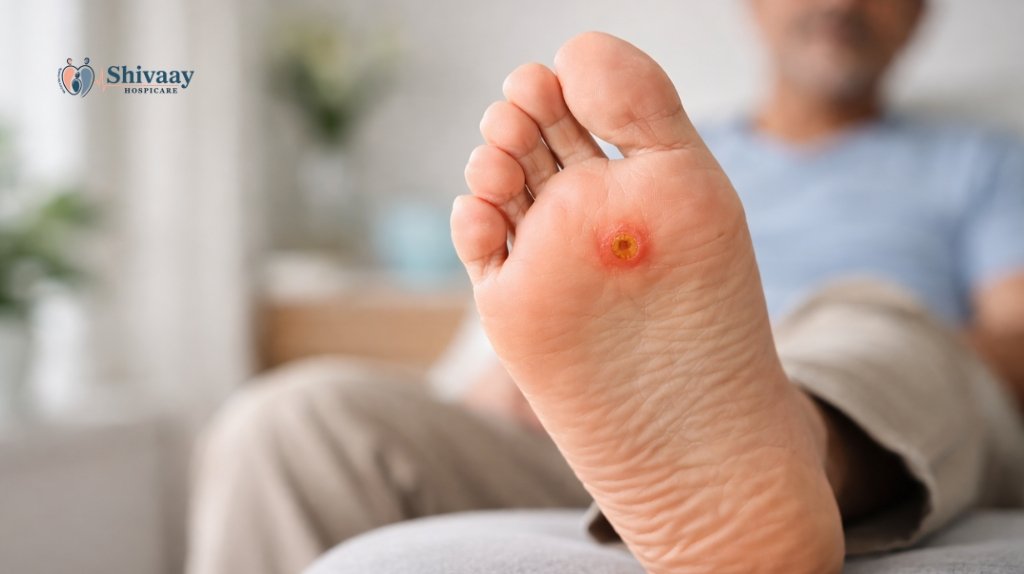
Type 2 diabetes, when not well controlled, can lead to several complications over time. One of the most serious and often overlooked complications is a diabetic foot ulcer. High blood sugar levels affect blood circulation, damage nerves, and weaken the body’s ability to fight infections.
Because of this, even a small wound on the foot can take weeks to heal and may worsen if not treated properly. In severe cases, it can lead to deep infections or even amputation.
Managing such cases requires more than just controlling blood sugar. A combination of proper wound care, infection control, lifestyle changes, and patient education plays a crucial role in recovery.
Patient Information
- Age/Sex: 55-year-old male
Chief Complaints:
- Non-healing ulcer on the left foot for 6 weeks
- Poorly controlled blood sugar levels
Medical History:
- Type 2 diabetes mellitus for 10 years
- Irregular use of prescribed medications
- Sedentary lifestyle
Current Medication:
- Oral anti-diabetic medicines (taken irregularly)
Clinical Presentation
The patient came with a persistent wound on his left foot that had not healed despite basic care. He reported:
- An open ulcer on the bottom (plantar surface) of the left foot
- Occasional fluid discharge from the wound
- Numbness in both feet
- Consistently high fasting blood sugar levels (above 200 mg/dL)
He did not recall any injury or trauma that could have caused the ulcer.
Clinical Examination
On examination, the following findings were noted:
- Ulcer Size: 3 × 2 cm
- Location: Plantar aspect of the left forefoot
- Wound Base: Presence of healthy tissue with some slough
- Surrounding Skin: Mild redness (erythema)
- Peripheral Pulses: Present (indicating blood flow was adequate)
- Sensation: Reduced, suggesting diabetic neuropathy
There were no signs of severe infection or systemic illness.
Diagnostic Assessment
Laboratory investigations revealed:
- Fasting Blood Glucose: 238 mg/dL
- Postprandial Blood Glucose: 320 mg/dL
- HbA1c: 10.2% (indicating poor long-term sugar control)
- CBC: Mild increase in white blood cells
- CRP: Elevated (suggesting inflammation)
- Kidney Function: Normal
- Wound Culture: Growth of Staphylococcus aureus (responsive to prescribed antibiotics)
Diagnosis:
- Uncontrolled Type 2 Diabetes Mellitus
- Diabetic neuropathy
- Non-healing diabetic foot ulcer
Therapeutic Intervention
A structured and step-by-step treatment plan was started to address both the root cause and the wound.
1. Glycemic Optimization
- Started on a basal-bolus insulin regimen for better sugar control
- Discontinued ineffective oral medications
- Educated the patient on regular blood sugar monitoring
- Advised a low glycaemic index diet
- Introduced a planned physical activity routine
2. Wound Management
- Surgical removal of dead tissue (debridement)
- Regular sterile dressing of the wound
- Antibiotics based on culture report
- Use of diabetic footwear to reduce pressure on the ulcer
3. Supportive Care
- Treatment for diabetic neuropathy
- Detailed education on daily foot care
- Weekly follow-up for wound assessment
Follow-Up and Outcomes
At 4 Weeks:
- Fasting blood sugar improved to 120–140 mg/dL
- Ulcer size reduced to 2 × 1.5 cm
- Healthy healing tissue visible
At 8 Weeks:
- HbA1c reduced to 7.8%
- Ulcer significantly smaller
- No signs of active infection
At 12 Weeks:
- Complete healing of the ulcer
- Improvement in numbness and nerve symptoms
- Better adherence to diabetes treatment and lifestyle changes
The patient did not require hospitalization and experienced no complications during treatment.
Discussion
High blood sugar levels over time can interfere with the body’s natural healing process. It affects:
- Immune response, making infections more likely
- Collagen formation, which is essential for wound repair
- Blood vessel function, reducing oxygen supply to tissues
- Nerve function, leading to unnoticed injuries
In this case, starting insulin therapy played a key role in quickly bringing blood sugar under control. This created a better environment for the wound to heal.
At the same time, proper wound care, infection control, and reducing pressure on the foot helped speed up recovery.
What made the biggest difference was a comprehensive approach, not just treating the wound but also addressing the underlying diabetes and patient habits.
Conclusion
This case clearly shows that non-healing diabetic foot ulcers can be successfully treated with timely and structured care. With proper blood sugar control, effective wound management, and patient education, complete healing is achievable.
Early intervention is critical. It can prevent serious complications, including infections and amputations.
Long-term follow-up and consistent diabetes management remain essential to avoid recurrence and maintain overall health.
Note: This case study is for illustrative purposes only and should not replace professional medical advice. If you have concerns about your health, please consult with a qualified healthcare provider.





